What is the Flu?
The Flu, also known as Grippe or Influenza is a respiratory infection caused by a number of possible viruses. The viruses pass through the air and enter your body through your eyes, ears, nose or mouth. Between 5% and 20% of people in the U.S. get the flu each year. The flu can be serious or even deadly for elderly people, newborn babies and people with certain chronic illnesses.
Symptoms of the flu come on suddenly and are worse than those of the common cold and may include:
- Body or muscle aches
- Chills
- Cough
- Fever
- Headache
- Sore throat
Take note: colds rarely cause a fever or headaches. Flu almost never causes an upset stomach. And "stomach flu" isn't really flu at all, but gastroenteritis.*
Read About Immune System Health...*
Steps to preventing a flu according to the CDC:
- Cover your nose and mouth with a tissue when you cough or sneeze. Throw the tissue in the trash after you use it.
- Wash your hands often with soap and water, especially after you cough or sneeze. Alcohol-based hand cleaners are also effective.
- Try to avoid close contact with sick people.
- If you get the flu, CDC recommends that you stay home from work or school and limit contact with others to keep from infecting them.
- Avoid touching your eyes, nose or mouth. Germs spread
this way.
Source: http://www.nlm.nih.gov/medlineplus, http://www.cdc.gov/flu/protect/preventing.htm
[Top]
More Information on Flu (Influenza)
Understanding Flu
Learn the basics about Flu (Influenza) from causes to complications. Here you will also find general publications, Spanish language information, and other fact sheets to download and print.
 |
|
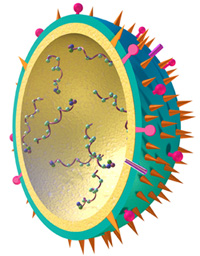
Flu virus Credit: NIAID |
- Flu Definitions & Overview
- Cause of Flu
- Flu Transmission
- Symptoms of Flu
- Flu Complications
- Diagnosis of the Flu
- Treatment of the Flu
- Flu Prevention
- Flu Publications
- 2009 H1N1 Flu
Flu Definitions & Overview
What's the Difference Between Seasonal Flu, Pandemic Flu, and Avian (Bird) Flu?
Influenza, or flu, is a respiratory infection caused by several flu viruses. Flu viruses are classified as types A, B, and C; type A has a number of subtypes. The flu is not the same as the common cold, nor is it related to what is commonly called the "stomach flu."
[top]
Seasonal Flu
Seasonal flu is the term used to refer to the flu outbreaks that occur yearly, mainly in the late fall and winter. It is estimated that between 5 and 20 percent of Americans come down with the flu every flu season.
[top]
Pandemic Flu
Pandemic flu refers to particularly virulent strains of flu that spread rapidly from person to person to create a world-wide epidemic (pandemic).
[top]
Avian (Bird) Flu
In nature, the flu virus also occurs in wild aquatic birds such as ducks and shore birds. It does not normally spread from birds to humans. However, pigs can be infected by bird influenza (as well as by the form of influenza that affects humans) and can pass on the flu to humans. In 1997, it was discovered that a virulent bird influenza had skipped the pig step and had infected humans directly, causing a number of deaths in Asia.
These instances of bird flu in humans have raised concerns that if this type of flu could at some point be transmitted between people, a new pandemic would occur. Thus, the term bird flu or avian flu is currently being used to refer to a possible pandemic flu.
[top]
Overview of the Flu
The flu, like the common cold, is a respiratory infection caused by viruses. But the flu differs in several ways from the common cold. For example, people with colds rarely get fevers or headaches or suffer from the extreme exhaustion that flu viruses cause. The most familiar aspect of the flu is the way it can "knock you off your feet" as it sweeps through entire communities.
The Centers for Disease Control and Prevention (CDC) estimates that 5 to 20 percent of Americans come down with the flu during each flu season, which typically lasts from November to March. Children are two to three times more likely than adults to get sick with the flu, and children frequently spread the virus to others. Although most people recover from the illness, CDC estimates that in the United States more than 200,000 people are hospitalized and about 36,000 people die from the flu and its complications every year.
[top]
Seasonal Flu Outbreaks
Seasonal flu outbreaks usually begin suddenly and occur mainly in the late fall and winter. The disease spreads through communities, creating an epidemic. During the epidemic, the number of cases peaks in about 3 weeks and subsides after another 3 or 4 weeks. Half of the population of a community may be affected. Because schools are an excellent place for flu viruses to attack and spread, families with school-age children have more infections than other families, with an average of one-third of the family members infected each year.
[top]
Importance of Flu
Besides the rapid start of the outbreaks and the large numbers of people affected, the flu is an important disease because it can cause serious complications. Most people who get the flu get better within a week (although they may have a lingering cough and tire easily for a while longer). For elderly people, newborn babies, and people with certain chronic illnesses, however, the flu and its complications can be life-threatening.
[top]
Flu Virus Characteristics
A flu virus is roughly round, but it can also be elongated or irregularly shaped. Inside are eight segments of single-strand RNA containing the genetic instructions for making new copies of the virus. Flu's most striking feature is a layer of spikes projecting from its surface. There are two different types of spikes: one is the protein hemagglutinin (HA), which allows the virus to "stick" to a cell and initiate infection, the other is a protein called neuraminidase (NA), which enables newly formed viruses to exit the host cell.
 |
|
Influenza A virus. Credit: CDC |
[top]
Virus Types A, B, C
Influenza viruses are classified as type A, B, or C based upon their protein composition. Type A viruses are found in many kinds of animals, including ducks, chickens, pigs, and whales, and also humans. The type B virus widely circulates in humans. Type C has been found in humans, pigs, and dogs and causes mild respiratory infections, but does not spark epidemics.
Type A influenza is the most frightening of the three. It is believed responsible for the global outbreaks of 1918, 1957, and 1968. Type A viruses are subdivided into groups based on two surface proteins, HA and NA. Scientists have characterized 16 HA subtypes and 9 NA subtypes.
[top]
Naming Viral Strains
Type A subtypes are classified by a naming system that includes the place the strain was first found, a lab identification number, the year of discovery, and, in parentheses, the type of HA and NA it possesses, for example, A/Hong Kong/156/97 (H5N1). If the virus infects non-humans, the host species is included before the geographical site, as in A/Chicken/Hong Kong/G9/97 (H9N2). There are no type B or C subtypes.
[top]
Where Influenza Comes From
In nature, the flu virus is found in wild aquatic birds such as ducks and shore birds. It has persisted in these birds for millions of years and does not typically harm them. But the frequently mutating flu viruses can readily jump the species barrier from wild birds to domesticated ducks and then to chickens. From there, the next stop in the infectious chain is often pigs.
Pigs can be infected by both bird (avian) influenza and the form of influenza that infects humans. In a setting such as a farm where chickens, humans, and pigs live in close proximity, pigs act as an influenza virus mixing bowl. If a pig is infected with avian and human flu simultaneously, the two types of virus may exchange genes. Such a "reassorted" flu virus can sometimes spread from pigs to people.
Depending on the precise assortment of bird-type flu proteins that make it into the human population, the flu may be more or less severe.
In 1997, for the first time, scientists found that bird influenza skipped the pig step and infected humans directly. Alarmed health officials feared a worldwide epidemic (a pandemic). But, fortunately, the virus could not pass between people and thus did not spark an epidemic. Scientists speculate that chickens may now also have the receptor used by human-type viruses.
[top]
Drifting and Shifting
Influenza virus is one of the most changeable of viruses. These genetic changes may be small and continuous or large and abrupt.
Small, continuous changes happen in type A and type B influenza as the virus makes copies of itself. The process is called antigenic drift. The drifting is frequent enough to make the new strain of virus often unrecognizable to the human immune system. For this reason, a new flu vaccine must be produced each year to combat that year's prevalent strains.
Type A influenza also undergoes infrequent and sudden changes, called antigenic shift. Antigenic shift occurs when two different flu strains infect the same cell and exchange genetic material. The novel assortment of HA or NA proteins in a shifted virus creates a new influenza A subtype. Because people have little or no immunity to such a new subtype, their appearance tends to coincide with a very severe flu epidemic or pandemic.
[top]
Causes of the Flu
The first flu virus was identified in the 1930s. Since then, scientists have classified influenza viruses into types A, B, and C.
- Type A is the most common and usually causes the most serious epidemics.
- Type B outbreaks also can cause epidemics, but the disease it produces generally is milder than that caused by type A.
- Type C viruses, on the other hand, never have been connected with a large epidemic.
[top]
Flu Transmission
You can get the flu if someone around you who has the flu coughs or sneezes. You can get the flu simply by touching a surface like a telephone or door knob that has been contaminated by a touch from someone who has the flu. The viruses can pass through the air and enter your body through your nose or mouth. If you've touched a contaminated surface, they can pass from your hand to your nose or mouth.
You are at greatest risk of getting infected in highly populated areas, such as in crowded living conditions and in schools.
[top]
Symptoms of Flu
If you get infected by the flu virus, you will usually feel symptoms 1 to 4 days later. You can spread the flu to others before your symptoms start and for another 3 to 4 days after your symptoms appear. The symptoms start very quickly and may include
- Body aches
- Chills
- Dry cough
- Fever
- Headache
- Sore throat
- Stuffy nose
Typically, the fever begins to decline on the second or third day of the illness. The flu almost never causes symptoms in the stomach and intestines. The illness that some call stomach flu is not influenza.
[top]
Flu Complications
You can have flu complications if you get a bacterial infection, which can cause pneumonia in your weakened lungs. Pneumonia also can be caused by the flu virus itself.
Complications usually appear after you start feeling better. After a brief period of improvement, you may suddenly get these symptoms
- High fever
- Shaking chills
- Chest pain with each breath
- Coughing that produces thick, yellow-greenish-colored mucus
Pneumonia can be a very serious and sometimes life-threatening condition. If you have any of these symptoms, you should contact your health care provider immediately to get the appropriate treatment.
Flu Complications In Children And Teenagers
Reye's syndrome, a condition that affects the nerves, sometimes develops in children and teenagers who are recovering from the flu. Reye's syndrome begins with nausea and vomiting, but the progressive mental changes (such as confusion or delirium) cause the greatest concern.
The syndrome often begins in young people after they take aspirin to get rid of fever or pain. Although very few children develop Reye's syndrome, you should consult a health care provider before giving aspirin or products that contain aspirin to children. Acetaminophen does not seem to be connected with Reye's syndrome.
[top]
Other Complications Of The Flu That Can Affect Children
- Convulsions caused by fever
- Croup
- Ear infections, such as otitis media
Newborn babies recently out of intensive care units are particularly vulnerable to suffering from flu complications.
[top]
Diagnosis of the Flu
Usually, health care providers diagnose the flu on the basis of whether it is epidemic in the community and whether the person's complaints fit the current pattern of symptoms. Health care providers rarely use laboratory tests to identify the virus during an epidemic. Health officials, however, monitor certain U.S. health clinics and do laboratory tests to determine which type of flu virus is responsible for the epidemic.
[top]
Treatment of the Flu
Health care providers can prescribe medicines to help fight the flu. These medicines are called antivirals and can be taken to treat or prevent the flu. For example, flu antivirals can be given to treat someone who just became sick (within 2 days). When the medicines are given to someone who is already ill, the symptoms and time the person is sick can be reduced. On the other hand, these same flu antiviral medicines can be given to a well person who has been in contact with someone who has the flu. Although this does not prevent you from getting the flu, it does reduce your chances of catching it and passing it on to others. By no means should these antiviral medicines be used in place of the flu vaccine.
Flu Drugs
Currently, there are four licensed antivirals against influenza A and B in the United States. However, only 2 of them are recommended by the CDC as a result of emerging influenza A resistance to the other two, amantadine and rimantadine:
- Tamiflu (oseltamivir) is for treating and preventing influenza A and B virus infections in adults and children 1 year and older.
- Relenza (zanamivir) is for treating influenza A and B virus infections in children 7 years and older and adults who have an uncomplicated flu infection and who have had symptoms for no more than 2 days. Relenza is also used to prevent flu infections in people 5 years and older.
For these medicines to work well, you must take them within 48 hours after the symptoms of flu appear. These medicines can reduce the length of time that a fever and other symptoms last, and allow you more quickly to return to your daily routine.
[top]
How Do Flu Drugs Work?
Zanamivir and oseltamivir are the first of a new class of antiviral drugs called neuraminidase inhibitors.
The surfaces of influenza viruses are dotted with neuraminidase proteins. Neuraminidase, an enzyme, breaks the bonds that hold new virus particles to the outside of an infected cell. Once the enzyme breaks these bonds, this sets free new viruses that can infect other cells and spread infection. Neuraminidase inhibitors block the enzyme's activity and prevent new virus particles from being released, thereby limiting the spread of the infection.
[top]
Who Should Consider Using These Drugs?
Antiviral medicines should be considered for people 1 year and older who want to be treated or avoid the flu and its complications. Health care providers should also consider those at high risk of flu complications. These medicines are an important step in fighting flu, but do not replace the best defense against the flu vaccine.
People allergic to these drugs or their ingredients should not take them.
Zanamivir generally is not recommended for people with chronic respiratory diseases such as asthma or chronic obstructive pulmonary disease (COPD). In clinical studies, some patients with mild or moderate asthma or COPD had bronchospasm (wheezing) after taking zanamivir. If you have an underlying respiratory disease and have been prescribed zanamivir, your health care provider should instruct you to have a fast-acting inhaled bronchodilator available for use when taking zanamivir.
The dosage of oseltamivir may need to be adjusted if you have any type of kidney disease.
None of these drugs is recommended for routine use during pregnancy or nursing. These drugs have not been evaluated in pregnant women, and researchers do not know the effects these drugs could have on the unborn child.
In the laboratory and in limited clinical studies, there have been no reported interactions of the neuraminidase inhibitors with other drugs.
For complete safety information about these drugs, talk with your pharmacist or health care provider.
[top]
How Much Do These Drugs Help?
Studies have shown that all four drugs can reduce the duration of flu symptoms by 1 day if taken within 2 days of the onset of the illness. There is no information about how effective these drugs are if treatment is started more than 2 days after the onset of flu symptoms.
When taken as directed to prevent the flu, oseltamivir can significantly reduce your chance of getting the disease if there is a flu outbreak in your family or community.
[top]
Flu Prevention
Flu Vaccine
The main way to keep from getting flu is to get a yearly flu vaccine. You can get the vaccine at your health care provider's office or a local clinic, and in many communities at workplaces, supermarkets, and drugstores. You must get the vaccine every year because it changes.
Scientists make a different vaccine every year because the strains of flu viruses change from year to year. Nine to 10 months before the flu season begins, they prepare a new vaccine made from inactivated (killed) flu viruses. Because the viruses have been killed, they cannot cause infection. The vaccine preparation is based on the strains of the flu viruses that are in circulation at the time. It includes those A and B viruses expected to circulate the following winter. More information about A and B viruses.
Sometimes, an unpredicted new strain may appear after the vaccine has been made and distributed. Because of this, even if you do get the flu vaccine, you still may get infected. If you do get infected, however, the disease will usually be milder because the vaccine will still give you some protection.
Until recently, you could get the flu vaccine only as an injection (shot). In 2003, however, the Food and Drug Administration (FDA) approved a nasal spray flu vaccine called FluMist that you can get from your health care provider. The FDA approved it for use in healthy people aged 2 to 49 years.
[top]
You Should Not Use FluMist If
- You have certain lung conditions, including asthma, or heart conditions
- You have metabolic disorders such as diabetes or kidney dysfunction
- You have an immunodeficiency disease or are on immunosuppressive treatment
- You have had Guillain-Barré syndrome
- You are pregnant
- You have a history of allergy or hypersensitivity, including anaphylaxis, to any of the parts of FluMist or to eggs
Children or teenagers who regularly take aspirin or products containing aspirin also should not take FluMist.
Your immune system takes time to respond to the flu vaccine. Therefore, you should get vaccinated 6 to 8 weeks before flu season begins in November to prevent getting infected or to reduce the severity of flu if you do get it. Because the flu season usually lasts until March, however, it's not too late to get the vaccine after the season has begun. The vaccine itself cannot cause the flu, but you could be exposed to the virus by someone else and become infected soon after you are vaccinated.
[top]
Possible Side Effects
You should be aware that the flu shot can cause side effects. The most common side effect in children and adults is soreness at the site of the vaccination. Other side effects, especially in children who previously have not been exposed to the flu virus, include fever, tiredness, and sore muscles. These side effects may begin 6 to 12 hours after vaccination and may last for up to 2 days.
Some people may opt for FluMist, the nasal-spray vaccine. Some side effects include runny nose, headache, cough, and fever.
Viruses for producing the vaccine are grown in chicken eggs and then killed with a chemical so that they can no longer cause an infection. The flu vaccine may contain some egg protein, which can cause an allergic reaction. Therefore, if you are allergic to eggs or have ever had a serious allergic reaction to the flu vaccine, the Centers for Disease Control and Prevention (CDC) recommends that you consult with your health care provider before getting vaccinated.
[top]
Vaccine Recommendations
If you are in any of the following groups or live in a household with someone who is, CDC recommends that you get the flu vaccine.
- Children and adolescents aged 6 months to 19 years
- Adults 50 years of age or older
- People with chronic diseases of the heart, lungs, or kidneys
- People with diabetes
- Those whose immune systems do not function properly
- People with a severe form of anemia
- Women who will be more than 3 months pregnant during the flu season
- People who live in a nursing home or other chronic-care housing facility
- Those in close contact with children 0 to 23 months of age
Health care providers and volunteers should get the flu vaccine if they work with people in any of the above groups.
Medicine for Prevention
Although the flu vaccine is the best way to prevent getting the flu, four antiviral medicines that will help prevent flu infection are also available by prescription. Two of these antivirals, amantadine and rimantadine, are no longer recommended because of documented influenza A resistance to them.
- Tamiflu (oseltamivir)
- Relenza (zanamivir)
Tamiflu may be used by adults and children who are 1 year of age and older. For people 5 years of age and older, Relenza is used to prevent the flu.
- These medicines help prevent the flu if you take them for at least 2 weeks during an outbreak of flu in your community.
- You may use these medicines if you are in close contact with family members or others who have the flu.
- You may use them if you are in close contact with people who have been vaccinated but whom you want to give added protection from getting the flu.
- You may use them immediately after being vaccinated during a flu epidemic to protect you during the 2- to 4-week period before antibodies develop, or when a flu epidemic is caused by virus strains other than those covered by the vaccine. (Antibodies are proteins from your immune system that protect you from the flu virus.)
Your health care provider can help you decide which medicine is best for you. You should discuss the flu vaccine and medicines with your health care provider before the flu season begins.
[top]
Source: http://www3.niaid.nih.gov/topics/Flu/understandingFlu/
2009 H1N1 Flu - NIAID 2009 H1N1 Influenza Research Program
NIAID support for influenza research over the past several years has greatly enhanced our preparedness for a pandemic influenza. The outbreak of the 2009 H1N1 influenza (swine flu) was unexpected; however, scientists in NIAID laboratories as well as NIAID grantees and contractors around the world have been studying diverse influenza viruses and are working to prepare for seasonal as well as pandemic influenza outbreaks.
Research on how influenza viruses replicate, interact with their hosts, stimulate immune responses, and evolve into new strains has created opportunities for new and improved design of influenza vaccines, diagnostic tools, and anti-influenza drugs. The research findings are applicable to seasonal epidemic and pandemic strains alike.
[top]
Basic Research
When news of the emergence of 2009 H1N1 influenza first broke, NIAID immediately began research on the virus in cell culture and in laboratory animals to identify the unique characteristics of the 2009 H1N1 virus.
NIAID-supported work includes research to better understand the biology of influenza viruses. For example, researchers are studying the evolution, adaptation, and pathogenesis of swine influenza viruses as well as how influenza viruses are transmitted between animals, from bird to swine or from swine to swine, from animals to human and between humans.
At the NIAID Centers of Excellence for Influenza Research and Surveillance (CEIRS), scientists conduct influenza surveillance in animals and study influenza pathogenesis and the host response to the influenza virus. Included in this research is domestic and international surveillance to collect, identify, and sequence the genomes of influenza viruses circulating in wild and domestic swine.
NIAID anticipates that these efforts will rapidly yield important information about which animals the virus can infect, the mechanisms by which the virus causes disease, the molecular signatures that indicate how virulent a virus strain may be and the major viral and host factors important in mounting an immune response to the virus.
[top]
Diagnostics
Quick and accurate tests for the diagnosis of an influenza infection are important for slowing the spread of the virus. Diagnostic tests are also important to help identify people who may have been infected with the 2009 H1N1 virus from people with other conditions who symptoms present like influenza. Rapid diagnostics also help to maximize the efficiency with which antiviral medications, such as those stored in the Strategic National Stockpile, are used.
NIAID has been developing diagnostic platforms capable of rapidly identifying a wide variety of pathogens in clinical samples, including specific subtypes of influenza, and the Institute is now working to accelerate development of these platforms to provide improved diagnostics for 2009 H1N1.
Antiviral Therapies
Antiviral medications are an important counterpart to vaccines as a means of controlling influenza and for treating infection after it occurs.
Although the currently circulating 2009 H1N1 virus is sensitive to oseltamivir (Tamiflu) and zanamivir (Relenza), experience tells us that resistance to influenza antiviral medications frequently emerges. Indeed, over the past two years the circulating seasonal H1N1 influenza viruses have become oseltamivir-resistant, even while other influenza viruses have remained sensitive to the drug.
In recent years, NIAID has been working to develop and test the next generation of influenza antivirals. Three drugs are now in clinical trials, including a long-acting neuraminidase inhibitor, an inhibitor of the enzyme that replicates viral genes, and a drug that prevents the virus from entering human lung cells. NIAID will soon begin to evaluate how well these candidate antiviral drugs block the 2009 H1N1 strain and to screen other compounds for activity against the virus.
[top]
Vaccine Research
| H1N1 Influenza Vaccine Development: A collaborative Process. View full-sized image. Credit: NIAID |
There are currently two types of licensed vaccines for prevention of influenza in the United States, inactivated vaccines that are based on chemically killed influenza viruses and injected intramuscularly; and live, attenuated vaccines that are based on a weakened influenza virus engineered to contain the genes of proteins, hemagglutinin and neuraminidase, of a circulating influenza strain and are given as a nasal spray.
The first step in creating both kinds of these vaccines for the 2009 H1N1 virus is the development of virus reference strains suitable for use in manufacturing. Once reference strains have been developed, they will be distributed to licensed manufacturers who will begin the process of producing limited quantities of vaccine known as pilot lots.
| NIH's Network of Vaccine and Treatment Evaluation Units (VTEUs). View full-size image. Credit: NIAID |
These pilot lots must be tested in clinical trials in humans before they can be approved for use by the FDA. The NIAID Vaccine and Treatment Evaluation Units (VTEU) will be used to quickly evaluate pilot lots of vaccine candidates to determine whether the vaccine is safe, induces protective immune responses, and the appropriate dose and number of dosages is determined. .
[top]
Flu Publications
Is It a Cold or the Flu?
¿Es un Resfrío o la Influenza?
Microbes: In Sickness and in Health
Understanding the Immune System
Understanding Vaccines: What They Are, How They Work
 Order Publications
Order Publications
Source: , http://www3.niaid.nih.gov/topics/Flu/understandingFlu/

 Get Well Natural, LLC
Get Well Natural, LLC  Kidney Function & Regeneration Health
Kidney Function & Regeneration Health  Platelet & Blood Cell Health
Platelet & Blood Cell Health  Prostate, Flow & Function Health
Prostate, Flow & Function Health  General Mind & Body Health
General Mind & Body Health  Heart, Cholesterol & Cardio Health
Heart, Cholesterol & Cardio Health  Allergy-Free Body
Allergy-Free Body  Anxiety & Stress
Anxiety & Stress  Blood Platelet Counts & Function
Blood Platelet Counts & Function  Blood Pressure Health
Blood Pressure Health  Kidney Health
Kidney Health  Immune System Health & Balance
Immune System Health & Balance  Prostate & Urinary Health Function
Prostate & Urinary Health Function  Blood Sugar Balance
Blood Sugar Balance  Cardiovascular Heart Health
Cardiovascular Heart Health  Detoxification & Healthy Cells
Detoxification & Healthy Cells  Women's Health
Women's Health  Liver Regeneration
Liver Regeneration  Pain-Free Body
Pain-Free Body  Water & Air Filtration
Water & Air Filtration 


